Artificial knee joint | Artificial knee
Knee prosthesis from a specialist
An artificial knee joint can fundamentally change the life of an affected person. It can relieve pain and restore mobility. However, the decision to have a knee replacement is a big one and requires weighing the pros and cons. Of course, since this procedure requires the necessary expertise, you want to be sure that you are being treated by an experienced surgeon who already has the expertise that this field requires, so that you can receive the best possible care.
I – Dr. Martin Gruber – have specialized in the medical treatment of knee pain and in the course of this have performed several thousand knee operations. In my practice in the MZA – the Alserstraße Medical Center – I have been treating patients of all ages, backgrounds and genders for years. Thanks to the latest surgical techniques and technologies, we can help you in the best possible way and find the most suitable therapeutic approach for you. In the course of this a first anamnesis is necessary – .
make an appointment for this in my office
.
What is meant by an artificial knee joint?
An artificial knee joint, also known as a knee prosthesis or colloquially as an “artificial knee”, is a replacement for a natural knee joint. In particular, it replaces the worn cartilaginous sliding and surfaces of the knee. It can be made of metal, plastic or ceramic and is inserted during surgery. In this procedure, the damaged, diseased parts in the knee joint are removed during surgery and replaced with the artificial implant. Depending on the extent of the osteoarthritis, either the entire knee joint is replaced (total knee arthroplasty), or only part of the affected joint section is replaced.
When do you need an artificial knee joint?
In some cases, my patients’ knee osteoarthritis has progressed to such an extent that it is no longer possible to achieve the desired healing stage with conservative therapies and the implantation of a knee prosthesis is unavoidable. Because osteoarthritis is a degenerative joint disease that worsens over time, the cartilage damage can become so extensive that conservative therapy (e.g., medication or physical therapy) does not improve symptoms.
If a patient with severe knee osteoarthritis still has problems after physiotherapy and “cartilage-building” therapy and no improvement in symptoms is seen, knee replacement must be considered.
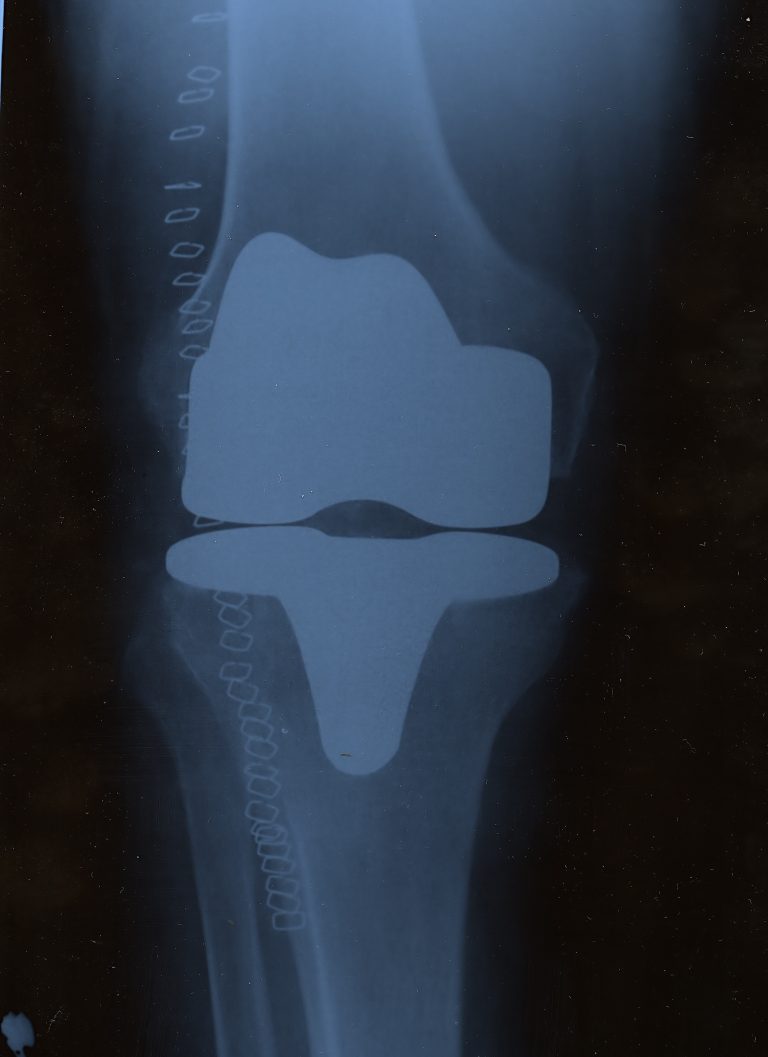
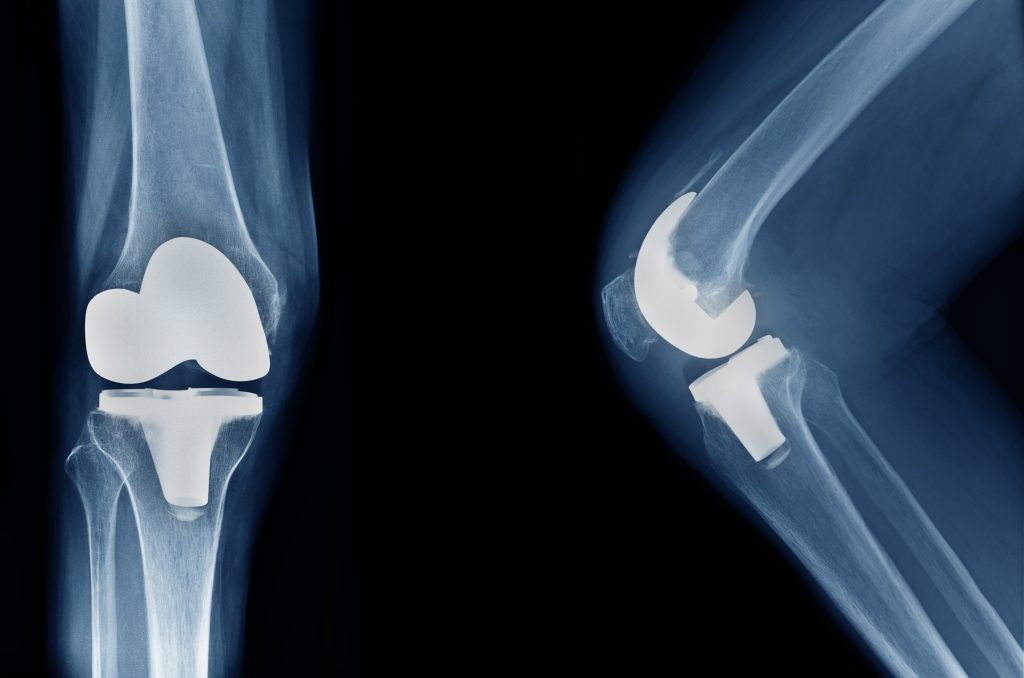
Clear indicators of the need for a knee prosthesis are the occurrence of night and rest pain, significant reduced mobility in the knee joint, and any associated discomfort that may interfere with pain-free management of everyday life. X-rays and MRIs are used to determine which parts of the knee need to be replaced and whether a knee arthroplasty is necessary. Such a clinical picture shows to what degree the cartilages are damaged and whether a knee prosthesis is necessary. The medical images from X-rays and MRIs help the treating orthopedic surgeon or knee specialist make a diagnosis and provide the information needed to decide how to proceed and choose the right knee prosthesis.
The most important indicators for the operation of an artificial knee joint at a glance:
- Severe knee pain that does not respond to conservative treatment
- Gradual deterioration of the knee joint due to wear and tear(osteoarthritis)
- Deformation of the knee joint due to rheumatoid arthritis
- Knee injuries that have not healed properly
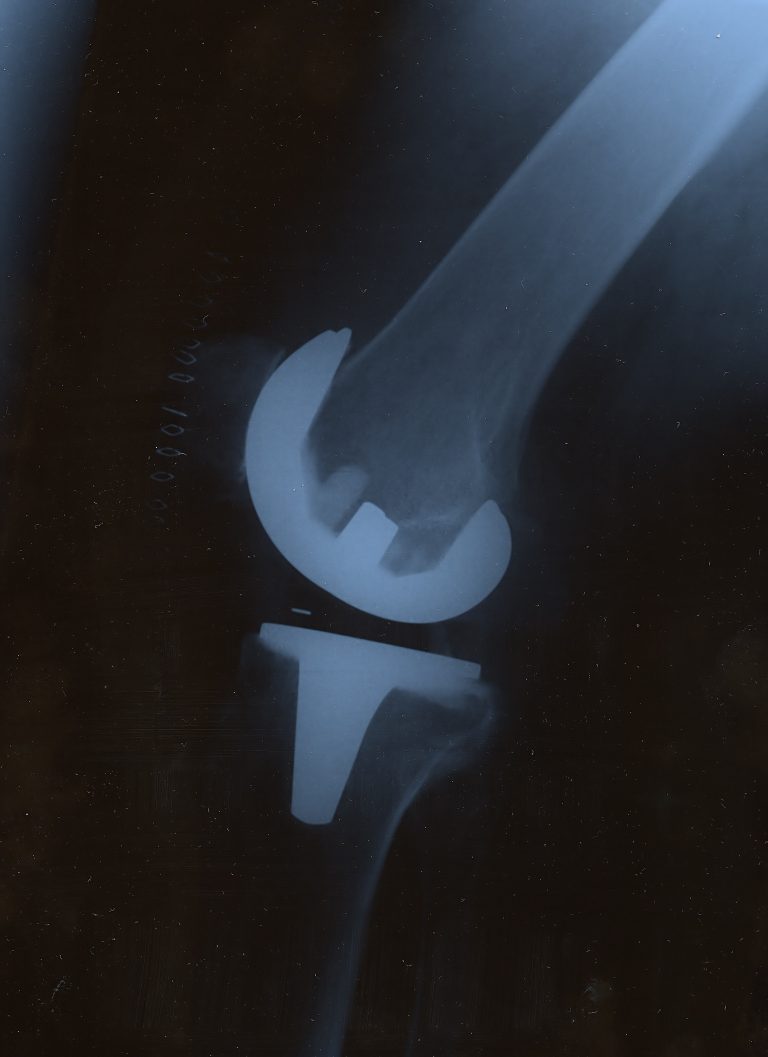
Prerequisites for the insertion of a knee prosthesis
In order to successfully insert a knee endoprosthesis, various factors must be considered in addition to the condition of the cartilage damage. Prerequisites for the insertion of an artificial knee joint are:
- That the patient is generally healthy and robust enough to withstand surgery
- that all local infections have been cured
- that there is no active inflammation in the area of the knee joint
It must also be ensured that the patient’s blood clotting function is normal and that there are no contraindications to general anesthesia. If these conditions are met, there is nothing standing in the way of knee surgery.
If you have any questions or would like to schedule an appointment, please contact me!
What is the procedure for artificial knee joint surgery?
The artificial knee joint is inserted during surgery. Depending on the extent of the damage to the knee joint, part of the knee may be replaced or it may be necessary to replace it completely. This decision is made by the attending physician based on X-rays and MRI scans prior to surgery.
If only a partial artificial knee replacement is required, only the damaged area of cartilage and bone is removed and replaced with an artificial implant. In this case, however, only one half or two thirds of the knee joint is replaced. Advantages of this procedure are that less bone tissue needs to be removed and that blood loss during surgery is significantly less. However, there is a risk that the artificial joint will become more worn over time and it may be necessary to replace the joint.
At the beginning of the procedure you will receive a general anesthesia and will not feel any pain during the procedure. The patient lies flat on his back in the operating room during this procedure. The skin is incised lengthwise in the midline of the leg, from slightly below the point where the Patellar tendon on the kneecap upwards to just above the point where the edge of the kneecap begins. To obtain a better view of the tibiofemoral joint, the patella is moved to the side after opening the joint. Then the diseased cartilage and bones of the knee joint are removed. In order to ensure a firm fit of the artificial knee joint, the implant is precisely adapted in size to the patient’s knee and fixed to the cut surfaces of the bone. At the end of the operation, the The stability and mobility of the knee prosthesis is checkedby moving the knee thoroughly to ensure the best possible result.
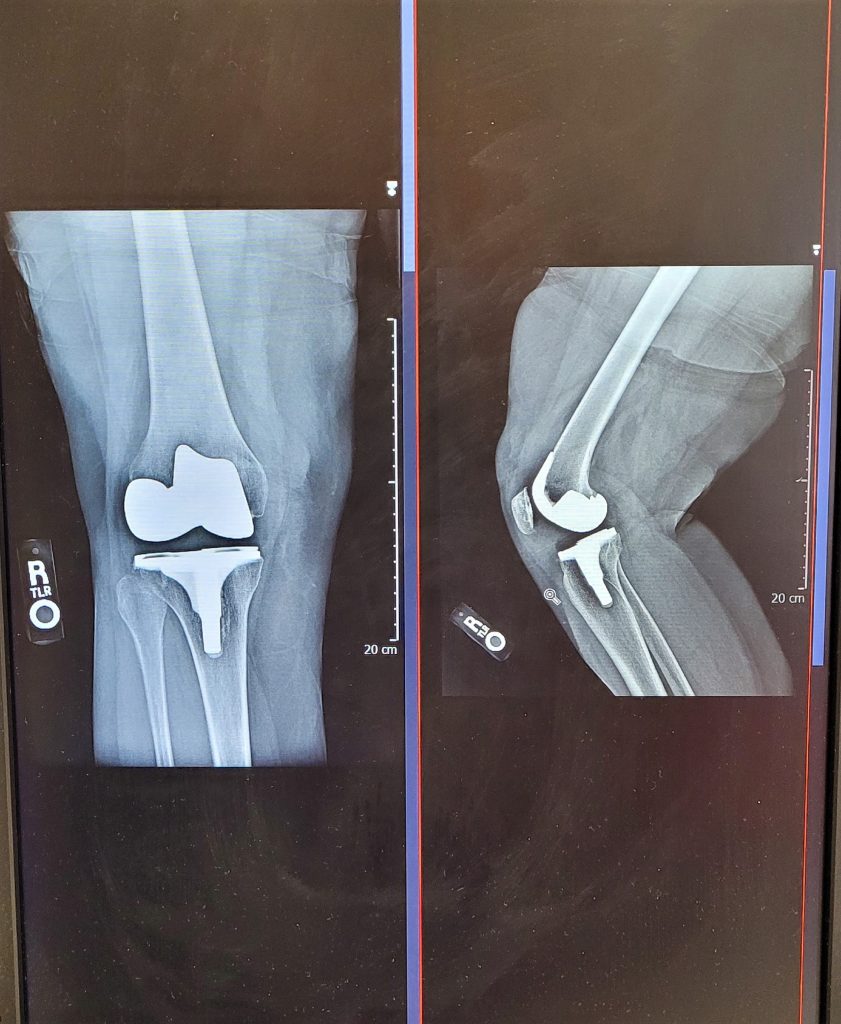
Options for knee replacement
Unicondylar surface replacement
If the joint surface is damaged only on one side of the knee, only this side is replaced. The advantages of this are that it is a much smaller procedure, the patient feels more natural about it, and healing occurs more quickly. Furthermore, this procedure is not an obstacle should a total surface replacement be necessary at a later date. The procedure is performed in a clinic.
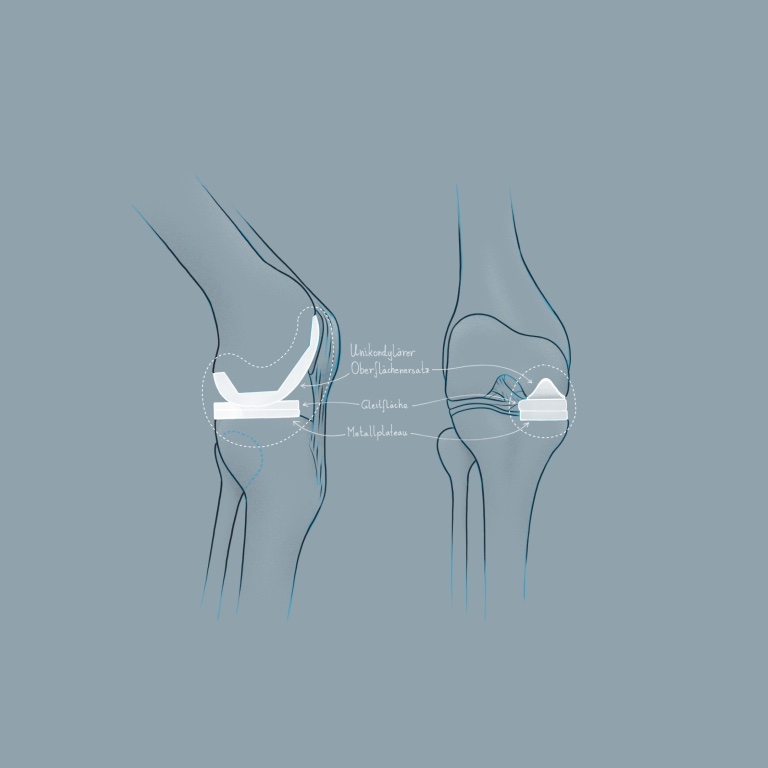
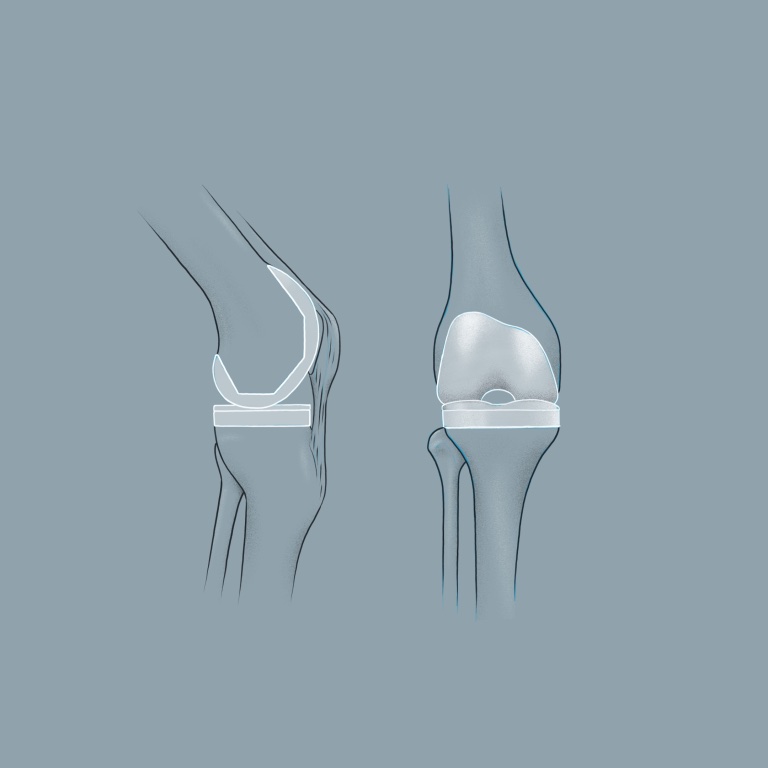
Bicondylar surface replacement
The entire sliding surfaces of the knee joint are replaced. The knee will be able to bear full weight again with the new surfaces after physiotherapy. In most cases, the decisive factor for success is not whether the latest generation of implants is used, but the surgeon’s knowledge of the ligament tension conditions within the knee joint and experience.
Artificial knee joint
The last resort for a broken knee is total knee replacement – the artificial knee. In this procedure, large parts of the joint are removed from both the lower and upper leg and a completely new joint is inserted. In medicine, artificial knee replacement is a very successful surgical procedureandis now widely used to drastically change the quality of life of the affected person(s). The joint replacement is made of metal and plastic. Here, the upper and lower leg components are made of metal, with the intervening sliding surface made of polyethylene. The knee prosthesis can additionally replace the kneecap.
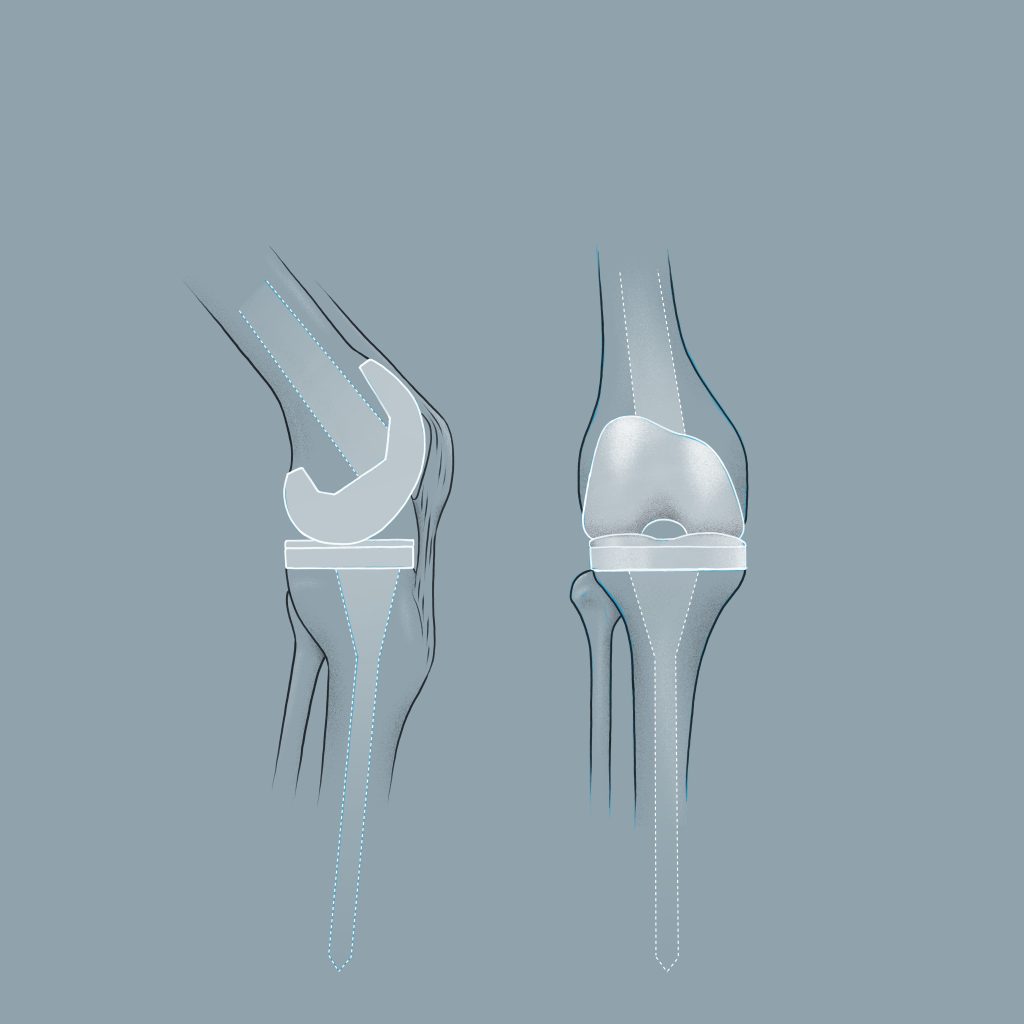
Are you looking for a knee specialist? Visit me in my practice at MZA – together we will find the most suitable therapy solution for you!
What are the risks and side effects of knee replacement?
As with any surgical procedure, there are certain risks associated with the use of the artificial knee joint. These include:
- Formation of blood clots and secondary bleeding
- Pain in the operated area
- Infections in the joint
- Dislocation of the knee endoprosthesis ("dislocation" or "loosening")
- Joint stiffening
Fortunately, the risk of inflammation after the insertion of a knee prosthesis is low and affects only one in a hundred patients operated on. To avoid possible risks, the instructions of the attending physician must be strictly observed!
What do I have to take into account after the operation of an artificial knee joint?
You will stay in the hospital or clinic for the first few days after surgery. During this time, the nursing staff will take care of you and make sure that your wound heals well and that you are pain-free. You will also receive physical therapy to help you regain strength and mobility in your knee as soon as possible.
It is important that you follow your doctor’s or physical therapist’s instructions carefully to ensure a successful outcome of the surgery. Depending on how well the healing process goes, you can expect to be discharged from the hospital within one to two weeks. After that, you should continue physical therapy at home or in an outpatient rehabilitation facility to ensure optimal rehabilitation and return to the old strength of your joints soon. It is important to move as much as possible to avoid stiffening the joint and surrounding muscles.
Aftercare after knee TEP summarized:
- Compliance with the predicted rest periods after the surgery
- Physiotherapy
- Massages
- (Underwater) gymnastics or strengthening training of the musculature
- Running and walking training to improve gait pattern
- Nutritional counseling
Is the operation of an artificial knee joint dangerous?
No, the operation of an artificial knee joint is not dangerous. However, there are always certain risks associated with surgery. These include: Infections, blood clot formation and secondary bleeding, deep vein thrombosis, nerve damage and blood clots. Joint stiffness is also a common side effect after surgery. Therefore, the stay in the clinic where the treatment was performed is inevitable after the operation. It is important that you follow your doctor’s or physical therapist’s instructions carefully to ensure a successful outcome of the surgery. Depending on how well the healing process goes, you can expect to be discharged from the hospital within one to two weeks. After that, you should continue physical therapy at home or at an outpatient rehabilitation facility.
Can you run/walk or do sports again with an artificial knee after the operation?
Yes, you will be able to run/walk or play sports again after surgery. However, for best results, it is important that you follow your doctor’s or physical therapist’s instructions carefully to ensure a successful outcome. During a surgery debriefing, you will be shown the recommended rest periods and explained when you can resume (intensive) sports. If you have concerns about whether you should participate in a particular activity, please consult your physician or physical therapist.
How long does an artificial knee joint (knee TEP) last?
The service life of an artificial knee joint depends on many factors, such as the patient’s age and weight, the type of activity the patient performs, and the quality of the implant. In general, however, most artificial knee joints can last 10 to 20 years. With proper care and maintenance, some patients can even extend the life of their artificial knee joint beyond 20 years.
Who performs knee arthroplasty surgery?
Knee arthroplasty is usually performed by an orthopedic surgeon. Often, the treating physician specializes in the knee and associated resurfacing.
"Tailor-made knee joint" for knee surgery
Dr. Martin Gruber explains what you should pay attention to during knee surgery!
Who performs knee arthroplasty surgery?
Who needs an artificial knee?
An artificial knee joint is often used in patients with advanced osteoarthritis or severe knee damage. If other treatments such as medications, physical therapy or injections do not provide adequate pain relief and knee mobility is severely limited, an artificial knee joint may be an option to reduce pain and restore mobility.
Will my knee pain go away with the use of a knee replacement?
There is a good chance that your knee pain will be significantly reduced after you have a knee replacement. The main purpose of a knee replacement is to relieve pain and improve the function of the knee joint. Many patients experience significant pain relief and improvement in mobility after surgery.
However, it is important to note that the success of pain relief and functional improvement depends on several factors, including the cause of your knee pain prior to surgery, the condition of the surrounding tissues and muscles, the degree of osteoarthritis or injury, and your individual healing process.
It is possible that some initial pain and discomfort may occur after the placement of a knee replacement, as the body needs time to adjust to the implant and heal the surrounding tissues. However, this is usually temporary and most patients experience continued improvement over time.
How long does an artificial knee joint last?
The lifespan of a knee prosthesis varies from patient to patient. As a rule, modern implants are designed to last 15 to 20 years or even longer. However, durability depends on several factors such as patient lifestyle, activity level, body weight and individual anatomy.
Can it happen that a knee prosthesis has to be changed?
Yes, in some cases it may be necessary to change a knee replacement. Although modern knee replacements are typically designed to last for many years, several factors can cause loosening, wear, or other problems that may require replacement of the prosthesis.
How long will I have to stay in the hospital after my knee surgery?
The length of hospital stay after knee surgery can vary depending on several factors, including the individual patient’s condition and the type of surgery performed. In general, the average length of stay after knee replacement surgery is about 3 to 5 days.
How long is the recovery time after knee replacement surgery
The recovery time may vary depending on the individual case. In the first weeks after surgery, rest and physiotherapeutic rehabilitation are important. Most patients require several months to fully regain mobility and strength. However, it may take up to a year to reach the full potential of your new knee replacement and return to your normal activities.
Can I play sports again with an artificial knee?
Yes, many patients with an artificial knee can return to sports after recovery and rehabilitation. However, the ability to participate in sports depends on several factors, including the condition of the knee joint, the type of sports activity, and the individual’s physical condition.
Moderate sports activities such as swimming, cycling, hiking, golfing or gentle jogging are usually well tolerated and can be resumed after successful knee replacement surgery. These activities provide a good way to improve fitness and strengthen the knee joint without putting excessive stress on the implant.
High-impact sports or those with quick, abrupt movements, such as tennis, soccer, basketball or skiing, can potentially be problematic with an artificial knee replacement. These activities may increase the risk of injury, overloading of the implant or premature wear. In some cases, your doctor may advise you not to participate in certain sports to preserve the life and function of the prosthesis.
How long is one unable to work after the insertion of a knee prosthesis?
The length of time you will be unable to work after knee replacement surgery can vary from patient to patient and depends on a number of factors, including the type of occupation, your overall health, your individual rate of recovery, and the recommendation of your treating physician.
As a rule, the average inability to work after knee prosthesis surgery is about 4 to 8 weeks. During this time, most patients need adequate recovery time to allow the surgical wound to heal, perform physical therapy exercises, and restore knee strength and mobility.
It is important to note that physically demanding jobs that require heavy physical labor or constant standing may require a longer recovery time. Your doctor will evaluate your individual case and make return-to-work recommendations based on your specific circumstances.
Are there any risks or complications associated with knee replacement surgery?
As with any surgical procedure, there are certain risks. Possible complications include infection, blood clots, injury to surrounding tissues and nerves, bleeding, and allergic reactions to anesthesia or implant materials. Your doctor will fully inform you about possible risks and complications before the surgery and take measures to minimize them.
Is the use of a knee prosthesis possible despite nickel allergy?
Yes, the use of an artificial knee is possible even if you are allergic to nickel. Modern knee prostheses are made of various materials, including metals such as titanium, cobalt-chromium alloys and also plastics. However, the use of nickel in knee prostheses has become relatively rare.
When is the right time for knee replacement surgery?
The right time for knee prosthesis surgery depends on various factors and should be done in close consultation with your treating physician. There are some general guidelines that are considered when deciding on a knee replacement:
Pain and dysfunction:
If you have persistent and severe knee pain that affects your quality of life and severely limits your range of motion, knee replacement may be considered. If conservative treatment methods such as medications, physical therapy or injections do not provide adequate relief, surgery may be considered.
Severe osteoarthritis:
Advanced osteoarthritis of the knee joint, characterized by wear of the cartilage and significant impairment of joint function, may be an indicator for knee replacement surgery.
Limitation of daily activities:
If your knee pain and dysfunction are affecting your ability to perform everyday activities such as walking, climbing stairs, or performing your job, a knee replacement may be considered to improve your ability to function.
Health condition:
Your overall health plays an important role in your decision to have surgery. Your doctor will evaluate your health and make sure you are suitable for the surgical procedure.
It is important to note that knee replacement is a treatment option that should only be considered after careful evaluation and discussion with your physician. Your doctor will evaluate your specific situation, weigh the pros and cons of surgery, and help you make the right decision for your individual case.
It is advisable to discuss all of your questions, concerns and expectations with your doctor in advance to get a clear understanding of the potential benefits, risks and outcomes of knee replacement surgery. all alternatives stand
